Māori healthcare ethics are grounded in Te Ao Māori (the Māori world view), emphasizing holistic well-being through principles like Manaakitanga (hospitality), Tino Rangatiratanga (self-determination), and Wairuatanga (spirituality). These ethics guide practitioners in fostering trust, ensuring cultural safety, and addressing health inequities by integrating traditional Rongoā Māori wisdom with contemporary clinical practices for better patient outcomes.
Understanding the Essence of Māori Healthcare Ethics
Māori healthcare ethics, often referred to within the broader context of Kaupapa Māori, represent a sophisticated and ancient system of values that predate Western clinical frameworks. At its core, these ethics are not merely a set of rules but a way of being and relating to the world. For the Māori, health (hauora) is not the absence of disease; it is the harmonious balance of physical, mental, spiritual, and family well-being. This perspective is famously encapsulated in the Te Whare Tapa Whā model, developed by Sir Mason Durie, which likens health to the four walls of a meeting house. If one wall is weak, the entire structure is compromised. In the clinical setting, Māori healthcare ethics demand a move away from the purely biomedical model toward a biopsychosocial-spiritual approach that respects the inherent dignity (mana) of every individual.
The application of these ethics is critical in addressing the historical and contemporary health disparities faced by Indigenous populations in New Zealand. By acknowledging the unique status of Māori as Tangata Whenua (people of the land) and the obligations under Te Tiriti o Waitangi (the Treaty of Waitangi), healthcare providers can create a more equitable system. This involves understanding that the patient is never an isolated individual but a member of a wider whānau (family), hapū (sub-tribe), and iwi (tribe). Ethics in this context become a collective responsibility, where the provider acts as a facilitator of healing rather than a sole authority.

Manaakitanga in Practice: Elevating the Standard of Care
Manaakitanga is frequently translated as hospitality, but in a clinical and ethical context, its meaning is far deeper. It is derived from the words ‘mana’ (prestige/authority) and ‘aki’ (to encourage or bolster). Thus, Manaakitanga is the act of uplifting the mana of others. In practice, this means treating every patient with extreme care, respect, and kindness. It begins the moment a patient enters a clinic. Is there a welcoming atmosphere? Is the provider prepared to engage in Whanaungatanga (relationship building) before diving into clinical questions? For many Māori patients, the quality of the personal connection determines the level of trust they will place in the medical advice given.
In a Rongoā Māori holistic lifestyle, Manaakitanga extends to how practitioners manage the environment. A clinic that embodies Manaakitanga will have spaces that accommodate whānau, acknowledging that the presence of loved ones is essential for a patient’s recovery. It also involves the ethical use of language and communication. Using Te Reo Māori (the Māori language) where appropriate, or even just correctly pronouncing names, is a powerful act of Manaakitanga that validates the patient’s identity. Clinically, this translates to higher patient satisfaction and better adherence to treatment plans, as the patient feels seen, heard, and valued as a human being rather than a case number.
Whanaungatanga: The Power of Connection
Whanaungatanga is the process of establishing links and making connections. In Māori ethics, the practitioner-patient relationship is not transactional. It is based on shared humanity. Practitioners who invest time in finding common ground—whether through shared geography, mutual acquaintances, or shared interests—are practicing ethical Māori care. This builds a foundation of ‘tautoko’ (support) that allows for more honest conversations about symptoms, lifestyle changes, and treatment barriers. In the absence of Whanaungatanga, a patient may withhold information due to a perceived lack of safety or cultural distance.
Tino Rangatiratanga and Patient Choice: Sovereignty in Health
Tino Rangatiratanga refers to self-determination, sovereignty, and autonomy. In the realm of healthcare, this is perhaps the most critical ethical principle for addressing power imbalances. For decades, the medical system operated under a paternalistic model where the doctor held all the power and knowledge. Māori healthcare ethics flip this script, asserting that patients have the right to be the architects of their own health journeys. This includes the right to choose traditional Māori healing (Rongoā Māori) alongside or instead of Western medicine without judgment or prejudice.
Ethical clinical integration requires that providers respect the patient’s agency. This goes beyond the Western concept of ‘informed consent,’ which is often a bureaucratic tick-box exercise. True Tino Rangatiratanga in a clinical setting involves ‘informed choice’ where the patient is given all relevant information in a way they understand, including the cultural and spiritual implications of their treatment. For example, when a Māori patient faces surgery, they may wish to have karakia (prayer) performed or to have body parts (such as the placenta or a removed gallstone) returned to them for burial. Respecting these choices is an act of acknowledging the patient’s Rangatiratanga over their own body and spirit.
Reclaiming Rongoā Māori
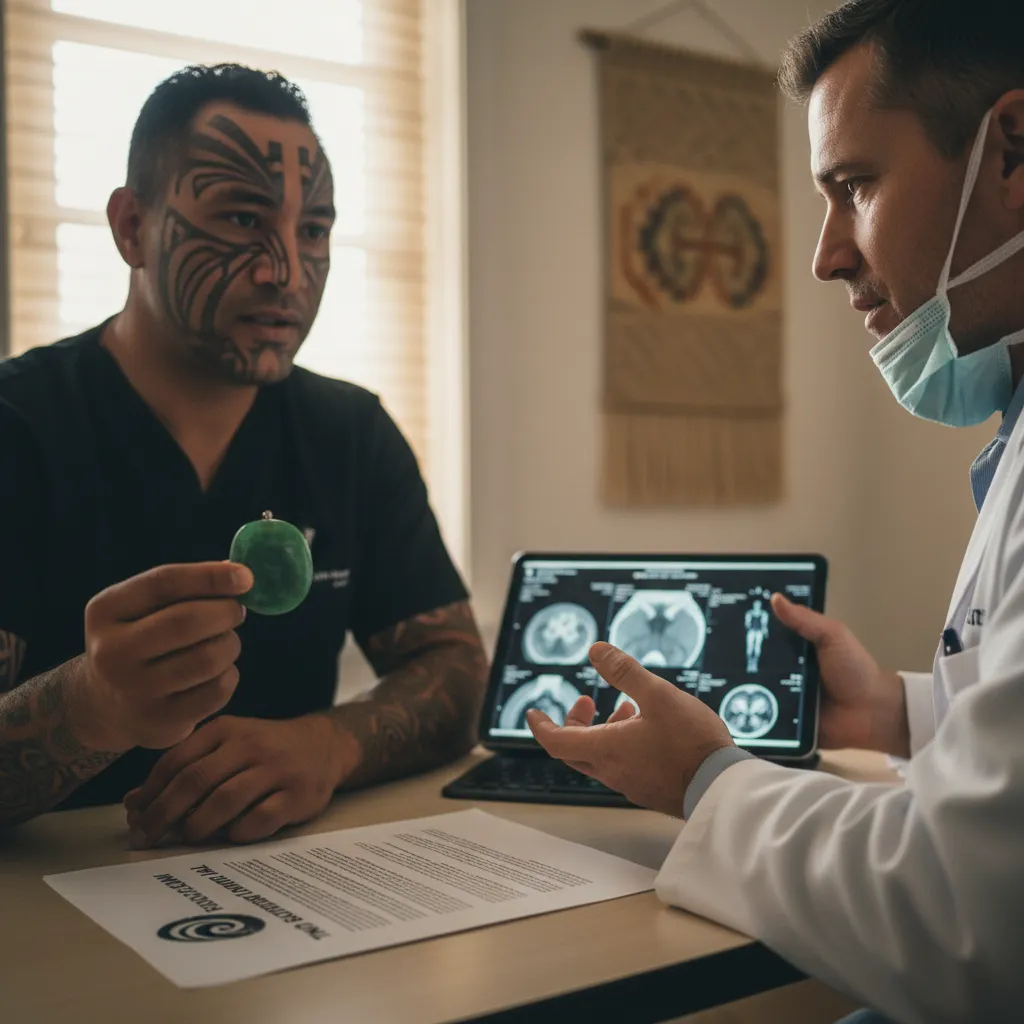
For many years, traditional Māori healing practices were marginalized and even outlawed by legislation like the Tohunga Suppression Act of 1907. Part of the ethical movement in modern healthcare is the reclamation and integration of Rongoā Māori. This is not just about using native plants for medicine; it is about recognizing the validity of an Indigenous knowledge system. Ethical practitioners today work in partnership with Rongoā practitioners, ensuring that the patient receives a seamless experience that honors both the physical and the metaphysical. This collaboration is a direct expression of Tino Rangatiratanga, as it allows Māori to define what ‘healing’ looks like for themselves.
Wairuatanga in Diagnosis: Addressing the Spiritual Dimension
Wairuatanga, or spirituality, is often the missing piece in Western medicine, yet it is considered the most essential requirement for Māori health. In Māori ethics, the spirit (wairua) is inextricably linked to the physical body (tinana). When a person is unwell, it is often seen as a symptom of a spiritual imbalance—perhaps a disconnection from one’s ancestors, the land, or a breach of ‘tapu’ (sacredness). Therefore, diagnosis in a Māori ethical framework must account for the state of the patient’s wairua. This does not mean a doctor must become a priest, but they must be open to the spiritual reality of the patient.
Ethically, this means creating space for spiritual practices within the clinical environment. It means not dismissing a patient’s feelings of being ‘unsettled’ as mere anxiety but exploring whether there are spiritual concerns that need addressing. For instance, a patient might feel that their illness is related to a historical grievance or a lack of connection to their ‘tūrangawaewae’ (place of standing). An ethical provider would support the patient in seeking spiritual guidance or performing rituals like karakia to clear the way for physical healing. Ignoring Wairuatanga is not just a cultural oversight; from a Māori perspective, it is an ethical failure that prevents holistic recovery.

The Sanctity of Tapu and Noa
Understanding the concepts of Tapu (sacred/restricted) and Noa (common/neutral) is vital for clinical ethics. Many parts of the body, particularly the head, are considered highly tapu. Touching a patient’s head without permission, or placing a hat on a table where food is served, is a breach of these ethical boundaries. Similarly, the transition from a state of tapu (such as being in a hospital or undergoing surgery) to a state of noa (returning to the community) requires careful management. Ethical care involves helping the patient navigate these states safely, ensuring that their spiritual integrity remains intact throughout the medical process.
Kaitiakitanga of Medical Knowledge: Guardianship and Data
Kaitiakitanga is the principle of guardianship and stewardship. While often applied to the environment, it is equally relevant to medical knowledge and patient data. In the context of Māori healthcare ethics, Kaitiakitanga involves the protection and careful management of Indigenous knowledge (Mātauranga Māori). This is particularly important when it comes to Rongoā Māori. The recipes for traditional medicines and the locations of sacred healing plants are collective intellectual property. Ethical practitioners must ensure that this knowledge is not exploited or commercialized without the express consent and benefit of the iwi or hapū from which it originates.
Furthermore, Kaitiakitanga applies to Māori data sovereignty. In an era of digital health records and genetic research, the question of who owns and controls Māori health data is a significant ethical issue. Māori data sovereignty principles argue that data about Māori should be controlled by Māori to ensure it is used in ways that support Māori aspirations and do not perpetuate negative stereotypes. An ethical healthcare provider or researcher must act as a ‘kaitiaki’ (guardian) of this data, ensuring transparency, security, and cultural safety in its handling. This prevents the ‘extractive’ model of research that has historically harmed Indigenous communities.

Ethical Research and Clinical Trials
When conducting clinical trials involving Māori participants, Kaitiakitanga requires a collaborative approach from the outset. This means involving Māori leadership in the design, implementation, and analysis phases of the research. It ensures that the questions being asked are relevant to Māori health priorities and that the results are shared back with the community in a way that is accessible and beneficial. This ethical stance moves research from being something ‘done to’ Māori to something ‘done with’ Māori, fostering a sense of ownership and trust in scientific advancements.
Clinical Integration and Cultural Safety
The integration of Māori ethics into clinical practice culminates in the concept of ‘cultural safety.’ Unlike ‘cultural competence,’ which focuses on the practitioner’s knowledge of other cultures, cultural safety focuses on the patient’s experience. A culturally safe environment is one where the patient feels that their identity and values are respected and that they are not being judged or coerced. This requires practitioners to engage in self-reflection (kōrero whakapapa) regarding their own biases and the historical power structures of the healthcare system.
To truly integrate Rongoā Māori and clinical care, institutions must move beyond tokenism. This involves hiring Māori health liasons, providing staff with ongoing training in Māori ethics, and redesigning clinical pathways to include Māori values at every stage. For example, a hospital might implement a ‘Whānau Ora’ approach, where the medical team works alongside a whānau worker to address the social and spiritual determinants of the patient’s health. This holistic integration ensures that the four walls of the patient’s ‘whare’ are all supported, leading to long-term wellness rather than just short-term symptom management.
Ultimately, Māori healthcare ethics offer a blueprint for a more compassionate, equitable, and effective medical system. By prioritizing Manaakitanga, Tino Rangatiratanga, Wairuatanga, and Kaitiakitanga, providers can bridge the gap between ancient wisdom and modern science. This not only benefits Māori patients but enriches the entire healthcare landscape, reminding us all that at the heart of medicine is the sacred duty to care for the whole person and their community.
People Also Ask
What are the 4 core Māori health values?
The 4 core values are Tinana (physical health), Hinengaro (mental health), Whānau (family well-being), and Wairua (spiritual health), often visualized as the four walls of Te Whare Tapa Whā.
How does Tino Rangatiratanga apply to medical consent?
It means patients have the right to self-determination, including the right to make informed choices about combining clinical treatments with traditional Rongoā Māori practices.
What is the role of Wairuatanga in modern nursing?
Wairuatanga involves acknowledging the spiritual needs of the patient, such as facilitating karakia (prayer) and respecting the sacred nature (tapu) of the patient’s body and identity.
How can non-Māori practitioners practice cultural safety?
By reflecting on their own biases, correctly pronouncing Māori names, building genuine relationships (Whanaungatanga), and respecting Māori protocols (tikanga) during care.
What is the difference between Rongoā Māori and western medicine?
Western medicine often focuses on physical symptoms and biochemical interventions, while Rongoā Māori is a holistic system using plant medicine, spiritual healing, and connection to the land.
Why is Whanaungatanga important in patient recovery?
Building a strong connection (Whanaungatanga) creates trust, which makes patients more likely to engage with their treatment and share critical health information with their provider.



